
What’s the current state of medical marijuana?
Author: Zoe Hill
Editor: Ellie Jackson
Artist: Vera Liu
Current social media is awash with ‘miracle’ cannabis-style treatments – a child experiencing uncontrollable epileptic seizures takes cannabidiol (CBD) oil and the seizure gradually subsides. Viewers are amazed, and left thinking – how? The number of CBD-based health products are rapidly increasing in availability on the UK high street. These products claim to relieve everything from anxiety to insomnia. So, why the hype? And why is a supposed miracle cure not available for prescription?
THC, CBD, and the Endocannabinoid system
CBD and delta-9-tetrahydrocannabinol (THC) are the two main compounds derived from the Cannabis Sativa plant. THC is psychoactive, causing the ‘high’ from recreational marijuana, and is more extensively researched than CBD. THC appears to alleviate symptoms of chemotherapy-induced nausea, tremors, and chronic pain. CBD is currently at the forefront of epilepsy research due to its potential as an anticonvulsant for drug-resistant epilepsy.
CBD and THC target the CB1 and CB2 receptors in the human nervous system, both have different properties of action and different distribution across the brain and peripheral nerves. Both of these receptors are indirectly involved in the regulation of neurotransmission in the brain, which produces changes that warrant a psychoactive effect.
Figure: CB1R and endogenous cannabinoid signalling
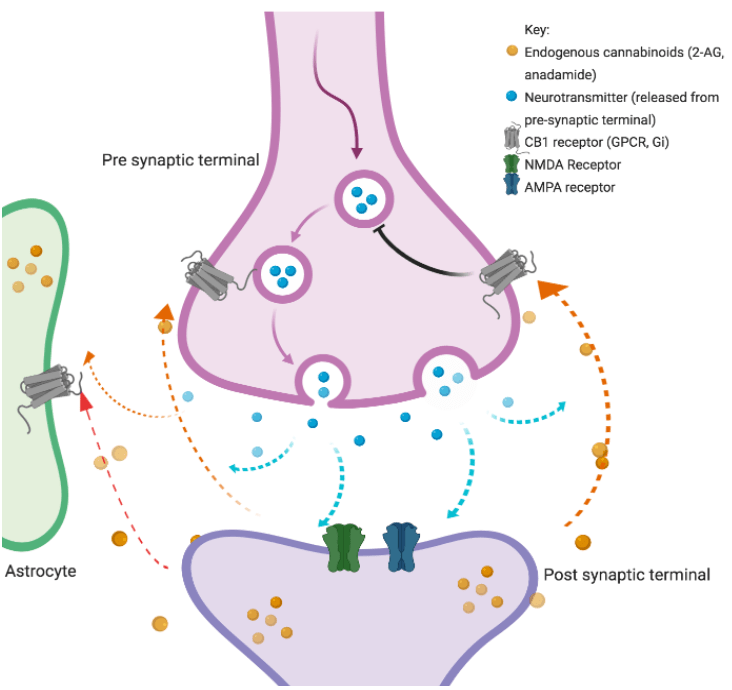
Figure 1: CB1 receptor activation caused by cannabinoids produced by the neuron. Cannabinoids are released into the synapse and target receptors on the pre-synaptic neuron and nearby cells such as glia and other neurons. Activation of these receptors is inhibitory, preventing the presynaptic neuron from sending responses onwards.
CBD and THC in use
The number of publications on medical marijuana is increasing each year, reporting positive efficacy of medical cannabis for different diseases. In its herbal form, the CBD to THC ratio is much lower and not regulated. Medical CBD currently prescribed on the NHS is typically a 20:1 CBD:THC ratio, limiting psychoactive side effects of THC. Some of the potential uses of medical marijuana are discussed below:
CBD as an anticonvulsant: Cases have reported dramatic seizure reductions as significant as 50 down to 2 a day. This reduction persists with continued CBD treatment, alongside weaning off of traditional anti-epileptics. This is particularly promising as it has been effective in drug resistant epilepsy, providing symptomatic relief from otherwise untreatable cases.
Reducing tremor: Herbal cannabis (non-prescription) is popular amongst sufferers of Parkinson’s disease. Research findings show that antagonising CB receptors helps to reduce tremor. If refined, such treatment could aid mobility and prevent patients having to take large doses of L-DOPA, the current drug used for Parkinson’s disease.
Chronic pain: Peripherally located CB2 receptors, when activated, could help to reduce stimulation from touch and reduce chronic pain. These effects could also occur in the central nervous system and help individuals with neuropathic pain, a disabling condition, find a new lease of life.
Medical Cannabis; now and the future
In the UK, cannabis is a class B drug, the group of ‘second most harmful and addictive illegal narcotics’. Despite its psychoactive effects, and concerns over the increasing strengths of the drug, a surge in cannabis research rocketed 5-10 years ago. Previously conducted trials show a positive relationship between medical cannabis and neurological symptomatic relief. However, the limitations of this research result in a lack of power to initiate legal change. Most clinical trials have small sample sizes and short follow-up periods, preventing the derivation of statistically significant conclusions. The new regulations of prescribing CBD-based treatments for drug-resistant epilepsy and chemotherapy-induced nausea are so constrictive, they limit prescription to patients that are legally entitled to the drug. Huge investment is required into research and policy before medical cannabis could become a readily accessible prescription drug.
The recognition of medical cannabis as treatment for neurological symptoms resistant to conventional drugs has undeniably increased in recent years. The drug can significantly improve quality of life for patients, potentially outweighing any harmful effects. However, we still lack a comprehensive understanding of how cannabis alleviates symptoms, and it’s potential links with the development of schizophrenia and other long-term health complications are still being explored. It is important to remember that medical cannabis is not a cure, but symptomatic relief. Much more vigorous, longitudinal research is required before any significant changes in regulations are likely to take place.
Sources
- Cannabinoid Receptors and the Endocannabinoid System: Signaling and Function in the Central Nervous System
- An Overview of the Cannabinoid Type 2 Receptor System and Its Therapeutic Potential
- The Case for Medical Marijuana in Epilepsy
- Ghovanloo, M. et al., 2018. Inhibitory effects of cannabidiol on voltage-dependent sodium currents.. J Biol Chem., 293(43), pp. 16546-16558.
- Ross, H., Napier, I. & Connor, M., 2008. Inhibition of Recombinant Human T-type Calcium Channels by Δ9-Tetrahydrocannabinol and Cannabidiol. Journal of Biological Chemistry, Volume 283, pp. 16124-16134
- Rodríguez-Muñoz, M. et al., 2018. Cannabidiol enhances morphine antinociception, diminishes NMDA-mediated seizures and reduces stroke damage via the sigma 1 receptor.. Molecular Brain, 11(1), p. 51.
- The Direct Actions of Cannabidiol and 2-arachidonoyl Glycerol at GABA A Receptors
- Cannabinoid type 1 receptor antagonism ameliorates harmaline-induced essential tremor in rat.
- Cannabinoids and Tremor Induced by Motor-related Disorders: Friend or Foe?
- Cannabinoids and Pain: New Insights From Old Molecules
- Amygdala activity contributes to the dissociative effect of cannabis on pain perception
- Medical cannabis in the UK
